A Pediatric Headache Specialist Shares Her Tips for Helping Kids Feel Better
Jennifer Dilts, a pediatric headache specialist, explores how kids experience headaches, what parents can do, and how families can get their lives back on track.

Jennifer Dilts, DO
Babies & Toddlers (0-2) Acute Pain Chronic Pain English Pain Management
Share this:

Do you need help with headaches right away?
Start here: the What the Heck Guide for headaches. Your step-by-step guide for what to do about your child’s headaches—when to worry, when to wait, and what actually helps.
Headaches can be confusing, stressful, and surprisingly common in children. Many families aren’t sure what’s normal, when to worry, or how to help their child feel better (especially when headaches start interrupting school, sports, or day-to-day routines).
This article brings together practical, evidence-informed guidance to help families understand what’s happening, why headaches occur, and what steps can truly make a difference. Throughout, you’ll find links to additional tools and resources designed to support families in recognizing patterns, managing symptoms, and building effective strategies together.
How common are headaches in kids and teens?
Headaches are far more frequent than many families realize. In fact, by age 15, more than 75% of children have experienced at least one significant headache. For migraines specifically, studies show about 11% of children ages 5–15 and nearly 28% of teens ages 15–19 are affected. Why does this matter? Because when headaches become frequent or severe they stop a child from playing, going to school, or spending time with friends. Migraines in particular often come with nausea, vomiting, and sensitivity to light or sound, making everyday life harder.
What types of headaches do kids get?
Kids and teens can experience several different types of headaches, and knowing which one your child has can help families and providers choose the most effective strategies. While every child is different, headaches generally fall into a few broad categories:
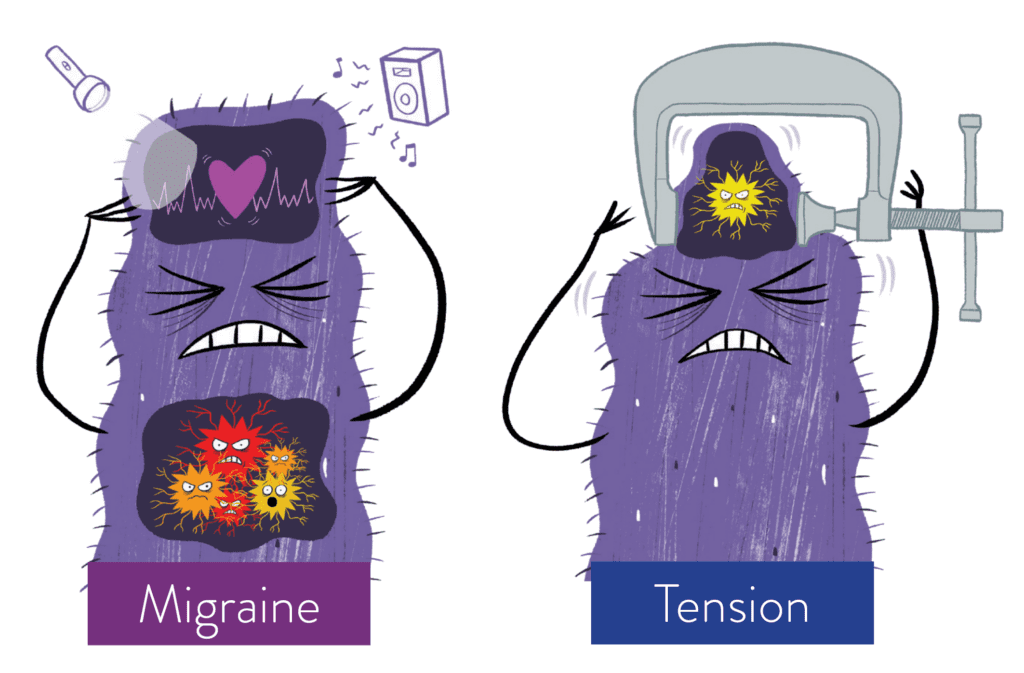
- Tension-type headaches – Often feel like pressure or tightness across the forehead or sides of the head.
- Migraines – Typically more severe, often with nausea, vomiting, or sensitivity to light, sound, or movement.
- Chronic headaches – When headaches happen very frequently or become persistent over time.
Because symptoms can overlap, it can be hard to tell which type your child is experiencing without support. Clear descriptions and tracking patterns can help your child’s provider understand what’s going on and guide the right next steps.
Not sure which type of headache your child is dealing with? Our Type of Headache Guide walks you through the differences so you can describe what’s happening more clearly to your child’s provider.
In the sections that follow, we’ll explore what triggers headaches, how they’re diagnosed, and what you can do to help your child feel better and return to the things they love.
What actually causes headaches in kids and teens?
Headaches are rarely triggered by a single factor—they’re most often the result of several things interacting. Some of the most common contributing factors include stress, sleep, weather changes, dehydration, nutrition, and more.
Because every child is different, identifying which triggers are most relevant to your child matters. That’s why tracking patterns over time can be so helpful—and why many headache specialists encourage families to use structured tools.
Keeping track of when headaches happen—and what was going on before they started—can reveal patterns you might not notice otherwise. Our Headache Diary makes it easy to record what matters and bring clear information to your child’s next appointment.


Family history also plays a strong role. Headaches often run in families, so if one parent has migraines, a child has a 50% chance of also having migraines. This number increases to around 75% if both parents have migraines. Understanding how headaches have appeared and evolved in your child (and potentially in other family members) can help your provider make a correct diagnosis.
Before your next appointment, our Headache History Form helps you pull together the details providers need most—family history, past treatments, and how your child’s headaches have changed over time.
Because headaches have many possible contributing factors, understanding the exact cause for your child often requires both tracking and teamwork. These tools help families gather clear, objective information that can be shared with clinicians, making it easier for providers to identify patterns, confirm triggers, and create an individualized plan that actually works.
What can families do to help kids with headaches?
The best thing families can do when headaches become a pattern is to work with a healthcare provider who understands pediatric headaches. Effective care is most successful when families can share clear, consistent information—and that’s where tools like the Headache Toolkit can make visits more productive and individualized.
At the same time, there are many everyday strategies that can help reduce the frequency and severity of headaches:
Build strong coping strategies for stress
Stress is a common trigger for headaches. Teaching kids simple coping strategies—like deep breathing, guided imagery, or relaxation exercises—can help calm their nervous system and prevent stress-related pain.

Manage Stress
Kids can learn to turn down pain and stress with practice. ImaginAction is an audio-guided tool that teaches calming strategies in a way that’s fun and age-appropriate—so kids can build confidence in managing how they feel.
Prioritize consistent sleep
Regular sleep and wake times support the brain’s ability to regulate itself. A calming wind-down routine and avoiding screens before bed can make a meaningful difference.

Stay hydrated
Regular hydration helps prevent some headaches. Many kids need more water than they realize, especially during sports or active days.
Eat regular, balanced meals
Stable blood sugar supports headache prevention. Encourage eating consistent meals and snacks. Limit caffeine intake to very occasional use.


Encourage daily movement
Physical activity releases endorphins—natural chemicals that help reduce pain and improve mood.
For many families, weaving these everyday habits into a consistent routine is the foundation of headache prevention.
Ready to put these everyday habits into action? Our Headache Prevention Action Plan helps your family build a simple, personalized routine—so you can focus on what’s working and adjust as you go.
When is it time to see a doctor for your child’s headaches?
If your child’s headaches are interfering with school, sports, sleep, or daily life, or if they’re happening once a week or more, it’s time to seek professional help. A visit with a pediatric headache specialist or your child’s primary care provider can help determine underlying causes, assess severity, and create a personalized care plan.

Helpful steps to prepare for the visit:
- Bring your completed Headache Diary—this gives the provider concrete data on the patterns, triggers, and frequency.
- Complete the Headache History Form ahead of time—knowing how headaches run in the family, what treatments have been tried, and how your child’s headaches behave helps the provider create a headache treatment plan that works.
- Fill out the Headache Symptom Checklist—a simple, structured way for families to note symptoms that accompany headaches—such as nausea, light sensitivity, dizziness, or sensory triggers. This helps providers quickly identify headache type and severity.
- Bringing this information to your child’s clinician puts you on the right path to finding a treatment plan that works!
Why is early treatment important for pediatric headaches?
When your child has a headache, “wait and see” is rarely the best approach. Treating headaches early—before pain becomes severe—can make rescue strategies more effective and help kids get back to their day more quickly. Medications like ibuprofen often work best when given at the first signs of a headache, not hours later.
Your child’s provider may also recommend rest in a dark, quiet room for a short period after taking rescue medication. Having a plan in place ahead of time (including keeping medication available at school when appropriate) can make these moments less stressful for everyone.
Building a strong offense: prevention + rescue plans
Rescue medications help once a headache starts, but a strong plan also includes prevention strategies that reduce how often headaches occur in the first place. For some kids, that may include preventive medications or supplements; for others, it may focus more on routines, sleep, hydration, nutrition, movement, and coping skills.
To keep everyone on the same page, many families find it helpful to write these strategies down, which is why we built these resources:
- Headache Prevention Action Plan — Helps families identify the daily habits, medications (if used), and supports that can reduce how often headaches occur.
- Headache Rescue Action Plan — Outlines the steps to take when a headache starts—at home, at school, or on the go—so kids and caregivers aren’t scrambling in the moment.
- Headache Action Plan Cheat Sheet — Shows real-world examples of prevention and rescue goals to help families personalize their plan.
- Headache Prevention & Rescue Strategy Overview — Summarizes strategies for prevention and rescue.
These tools make it easier for kids, caregivers, and providers to respond consistently on both good days and tough ones.
What non-medication treatments can help with pediatric headaches?
In addition to medications and supplements, there are several evidence-based approaches that can help kids manage headaches. These options can be especially helpful for families who want non-medication strategies or who need additional tools alongside their care plan.
Some treatments that providers may recommend include:
- Hypnosis — Helps kids develop deep relaxation and self-regulation skills.
- Acupuncture — Can reduce pain and help with overall symptom management.
- Biofeedback — Teaches kids how to understand and control certain body responses tied to stress and pain.
- Cognitive behavioral therapy (CBT) — Helps kids build coping strategies, reduce stress, and address thinking patterns that may intensify pain. (See The Comfort Ability Program for a CBT-based workshop program.)
- Neurostimulation devices — Certain devices can prevent headaches and/or provide relief during pain episodes.
These approaches can be used on their own or in combination with medications. The right fit depends on the child, their symptoms, and their provider’s recommendations.
It’s powerful to know that while headaches are nobody’s fault, there are many ways to take control of the pain experience. Partnering with your child’s provider—and bringing tools and information—helps you build the combination of strategies that works best for your child.
If you’re looking for simple, evidence-informed tools that can support your family, our Headache Toolkit brings everything together in one place—tracking worksheets, symptom guides, prevention and rescue plans, and practical strategies for everyday support.
Headaches don’t have to define your child’s life. With information, planning, and support, kids can stay engaged in the things they love.
You May Also Be Interested In

Downloads
Test: Provider ToolKit
This interactive eBook makes it easy to learn all the ways our free pain management resources can be used to make life easier for you and your patients.
Downloads
Child Life Specialists Poster
An illustrated guide to the people who help kids cope through some of the hardest moments in healthcare — who they are, what they do, and why every family should know to ask for one.

About the Author
Dr. Jennifer Dilts is a pediatrician and medical acupuncturist at Bloom Pediatrics in Kansas City, Kansas. Prior to moving to private practice in 2023, she was the director of Children’s Mercy Kansas City’s Comprehensive Headache Clinic and an associate professor of pediatrics at the University of Missouri-Kansas City. She is board-certified in pediatrics, headache medicine, and medical acupuncture. Her pediatric acupuncture research has won several grants and national awards. Additionally, she has designed a curriculum to teach optimal procedural pain and anxiety management to pediatric residents. As the mom of three daughters, she feels passionately about empowering kids before and during procedures. She also loves talking with kids and teens about headaches, ADHD, and mental health.




